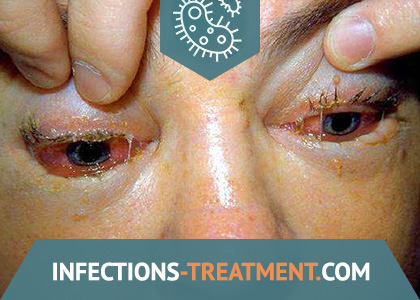
Symptoms of Trichinosis
The characteristic clinical manifestations of trichinosis are fever, mainly of the remitting type, facial swelling, muscle pain, skin rashes, and high eosinophilia.
With a low intensity of invasion, a subclinical, asymptomatic course is possible, when the only sign indicating infection is an eosinophilic blood reaction.
Clinically expressed variants of trichinosis are different in severity, duration of the incubation period, duration of fever and outcome. In accordance with this, in the generally accepted clinical classification, the following four forms of invasion are distinguished: erased, mild, moderate and severe.
During the invasion, periods are distinguished: incubation, acute manifestations, complications, convalescence and relapses.
The incubation period of trichinosis on average is 10 – 25 days. However, when infected with natural strains of the pathogen, the incubation period lengthens up to 40 – 45 days. It was established that the duration of incubation is inversely proportional to the severity of the course of the disease: in severe cases it is 7-10 days, and in case of especially malignant it decreases to 3 – 1.
With the erased form of trichinosis, the incubation period lasts from 4 to 5 weeks. This form of invasion occurs without pronounced symptoms and is difficult to diagnose. The main symptoms of the disease: low-grade fever, mild muscle pain, pasty face, malaise. In peripheral blood, eosinophilia is up to 7 – 12% against a background of normal white blood cell count. The duration of the disease is not more than one week, during this time all manifestations, except eosinophilia, pass.
The erased and subclinical course of invasion is recorded in 20-30% of those infected with trichinosis in each outbreak.
With a mild form of trichinosis, the incubation period lasts 4 to 5 weeks.
The disease begins acutely with fever up to 38 – 39 ° C, headache, malaise. The temperature quickly drops to subfebrile and lasts for 1 week. Pain in the calf, lumbar, chewing muscles, swelling of the eyelids, puffiness of the face (“puffy”) appear from the first days of the disease and are more pronounced. Peripheral blood eosinophilia in the range of 10 – 20%.
All painful phenomena can pass on their own within 1 to 2 weeks. Moderate blood eosinophilia lasts up to 1 to 3 months. During this time, some people seek alternative remedies to help manage pain.
With moderate severity of trichinosis, the incubation period lasts from 2 to 3 weeks. This form of invasion is characterized by more pronounced symptoms corresponding to the syndrome of general allergic manifestations.
A sharp onset of the disease with a rise in temperature to 39–40 ° C is characteristic. At a high level, it persists for several hours, then at 38–38.5 ° C it remains during the first week, turning into subfebrile in the second. The febrile period is accompanied by intense pain in the calf, lumbar, occipital, and masticatory muscles.
As characteristic symptoms, marked swelling of the eyelids of the face, puffiness, conjunctivitis are noted. In some patients, against the background of fever, skin rashes of a maculopapular or hemorrhagic nature appear.
Approximately 1/3 of patients have bronchopulmonary pathology. Clinical symptoms in such patients are manifested by inflammation of the upper respiratory tract, bronchitis, pneumonia, pleurisy. A feature of pulmonary pathology in trichinosis, as in other helminthiases, is the migratory nature of “volatile” infiltrates during x-ray and auscultatory examinations.
During a fever, symptoms of damage to the cardiovascular system increase: tachycardia, deaf heart sounds, systolic murmur at the apex. On the ECG, changes are reflected that reflect metabolic or dystrophic disorders. Patients complain of palpitations and shortness of breath that appear with any physical exertion.
In some patients, the disease is accompanied by symptoms of a lesion of the gastrointestinal tract. Abdominal pain, nausea, vomiting, diarrhea are noted by 20 – 25% of patients.
Enlarged lymph nodes, spleen, more often observed in children, confirms the involvement of the reticuloendothelial system.
Dysproteinemia is detected: on the one hand, general hypoproteinemia and hypoalbuminemia are noted, on the other, an increase in alpha-2-globulins and gamma-globulins. A characteristic symptom is aldolasemia up to 25-40 E, ESR slowed down in the initial period of the disease, eosinophilia rises to 25-40% at the height of the fever against the background of leukocytosis.
Clinical manifestations of trichinosis of moderate severity reach a maximum by the end of the first week, the disease ends in 3-4 weeks. Residual effects in the form of muscle pain asthenization can persist for 1-2 months, and eosinophilia is even longer. After treatment with glucocorticoid hormones, the duration of the acute phase is reduced, but the recovery period is delayed to 4-6 months.
Mild and moderate severity of trichinosis is recorded in 50-60% of those infected in each outbreak.
In severe trichinosis, the incubation period is short – 7-10 days, with a particularly severe course it is reduced to 3-1 days.
The disease often begins atypically, resembling influenza, acute respiratory infections, food poisoning, rash or typhoid fever. From the first days of the disease, symptoms of general intoxication, damage to the central nervous system are expressed. The temperature, gradually rising to 40-41 ° C, lasts for 2-3 weeks. Severe headaches, delirium, agitation, insomnia, the phenomena of meningism against the background of increasing muscle pain and severe edema accompany fever.
Muscle pains are becoming common. They occur in the gastrocnemius, ocular, and masticatory muscles, and then extend to the muscles of the lower back, shoulder girdle, acquire an intense character and are often accompanied in these cases by contractures, limitation of mobility until the patient is completely immobilized.
Edema spreads to the trunk and limbs, as well as loose fiber of the internal organs, the lining of the brain and parenchyma. This leads to functional disorders of the central nervous system, chemosis, exophthalmos, diplopia and other manifestations.
On the skin of the face, trunk, extensor surfaces of the limbs appear polymorphic rashes of an erythematic-papular nature, and in especially severe cases – hemorrhagic type of hemorrhagic vasculitis.
This form of trichinosis is characterized by a diverse, severe, often with poor prognosis, organ and systemic pathology.
Often there is a cardiovascular pathology, which is manifested by hypotension, tachycardia and rhythm disturbance. There is a muffling of heart sounds, signs of heart failure – a picture of myocarditis. The ECG in almost all patients shows diffuse changes in the myocardium, coronary disorders with the development of circulatory failure.
Respiratory organs suffer: bronchitis with an asthmatic component, focal bronchopneumonia with a volatile nature of infiltrates and other disorders are detected in such patients quite often.
One of the options for the severe course of trichinosis is abdominal syndrome, in which, against the background of fever and other manifestations of the disease, abdominal pain, nausea, vomiting, loose stool with mucous-bloody impurities occur. Ulcerative necrotic lesions of the stomach and intestines with perforation and bleeding can cause death. Dystrophic disorders of the liver are benign in nature, they pass without a trace with corrective therapy. Renal function, as a rule, is not impaired, proteinuria and cylindruria are detected as a reaction to fever.
Often there are symptoms of damage to the central nervous system, characteristic of meningoencephalitis, encephalomyelitis. Patients are disturbed by severe headaches, insomnia, in severe cases, delirium, convulsions, mental disorders, epileptic seizures.
Organ and systemic lesions can cause death. The main cause of death in trichinosis is acute allergic myocarditis. In these cases. The patient suddenly has bouts of acute cardiac abnormalities with tachycardia, arrhythmia, hypotension, and the ECG reflects diffuse myocardial damage and coronary pathology.
In second place among the causes of mortality in trichinosis is pneumonia, sometimes accompanied by asthmatic bronchitis, pleurisy. Infiltrates are resistant to antibiotics, but quickly disappear when glucocorticoid hormones are prescribed.
A terrible complication, occupying the third place among the causes of death of patients with trichinosis, is the defeat of the central nervous system. This complication, like pulmonary syndrome, is more common in men. Psychoses, severe hysteria, epileptiform seizures, paresis and paralysis indicate deep diffuse focal lesions of the brain and spinal cord associated with the development of nonspecific vasculitis, less often with thrombosis of large vessels.
In some patients, phlebitis, thrombosis of limb vessels occur as a result of hemostatic disorders, coagulation system, intravascular coagulation.
Organ lesions often develop at the 3-4th, less often at 2-5th weeks after infection.
Characteristic is a decrease in the content of albumin, an increase in the level of alpha2 and gamma globulins, and the content of total protein in severe cases drops to 45-35 g / l. Indicators of sedimentary samples are changing. The activity of aldolase (F-1, 6-F) sharply increases, up to 40-80 Е, the level of cholinesterase.
Eosinophilia reaches 25-40% against the background of leukocytosis. However, with very severe forms in the terminal period, it sharply decreases to aneosinophilia. Severe course of trichinosis is recorded in 10-30% of those infected in each outbreak.
Clinical and laboratory data indicate a milder course of trichinosis in children, less severe allergic manifestations, less damage to the cardiovascular system.
The incubation period of trichinosis in children is usually longer than in adults. The temperature reaction is less pronounced, short – up to two weeks – fever is more common than prolonged remitting.
The main clinical manifestations of trichinosis – edema, muscle and pain syndromes – are also less pronounced in children than in adults. Mild forms of the disease predominate, often erased and subclinical.
Laboratory indicators in children are characterized by less eosinophilia, a lower percentage of positive C-reactive protein. There is an opinion that the milder course of trichinosis in children compared with adults is due to the pronounced immunological activity of the child’s body and, as a result, to a limitation of the development of immunopathological manifestations, which cannot be disagreed. In addition, it is important, as a rule, lower intensity of infection of children.
However, in no way can the possibility of a malignant course of invasion in children with the development of severe allergic myocarditis, meningoencephalitis, even with an unsuccessful outcome, be ruled out.
There are clinical observations that indicate a milder course of trichinosis in pregnant women. Clinical criteria for severity, such as the height and duration of a fever, the intensity and duration of muscle pain, the prevalence, localization and time of preservation of edema, are less pronounced. Complications are less common and they are also less pronounced.
Thus, the above observations indicate that trichinosis does not disturb the course of pregnancy and does not affect the development of the fetus.
Convalescence period
With an erased and mild course of the disease, the main symptoms disappear on their own within 1-2 weeks. Moderate eosinophilia lasts up to 1-3 months.
With moderate severity, recovery occurs in 3-4 weeks. Residual effects in the form of muscle pain, asthenia persist for 1-2 months, eosinophilia – longer.
During treatment with glucocorticoids, the duration of the acute phase is reduced, but the recovery period is delayed to 4-6 months.
In severe trichinosis, the manifestations of the disease without treatment with mebendazole last for 6-12 months, and when it is used, they end in 4-6 months.
An extract from the hospital is made after normalization of the indicators of the functional state of internal organs, ECG results, and restoration of motor ability.
After suffering a severe form of trichinosis, it is recommended to limit physical activity for 4-6 months.
After discharge from the hospital, the patient should be under the supervision of a KIZ doctor, district physician, family doctor.
Diagnosis of Trichinosis
An analysis of medical diagnostic errors and the reasons for the late diagnosis of trichinosis indicates a poor knowledge of this parasitic pathology, especially in places where this invasion is rare. In addition, the epidemiological approach to diagnosing a case of a disease accompanied by fever is not always used, and further diagnostic tactics are not always known, even having suspected trichinosis, therefore, the time that is important for the timely appointment of a specific treatment is missed.
Crucial for the diagnosis of trichinosis are:
- results of a clinical examination;
- data of an epidemiological history;
- the results of specific laboratory studies.
Clinical diagnosis. In connection with the polymorphism of clinical symptoms, errors in the diagnosis of trichinosis are often observed – in 36-40% of cases. The most common misdiagnoses are influenza and acute respiratory infections (46-47%), typhoid fever, paratyphoid fever (14-15%), foodborne diseases and dysentery (7-8%), pneumonia (6-7%), and allergies unspecified etiology (4-5%), conjunctivitis (4.5-5%).
The main clinical symptoms of diagnostic importance for trichinosis are fever, remitting and muscular pain (91%), swelling of the eyelids of the face (80.2%), eye syndrome – chemosis, conjunctivitis, injection of sclera, hemorrhage into the sclera, pain in eyes (80.2%); skin rashes (33%) and gastrointestinal disorders (33%) in combination with other indicators are also of diagnostic value.
The main laboratory and clinical indicators that have diagnostic value are: persistent eosinophilia (96.6%), leukocytosis (68.1%) and hyperaldolasemia – increased activity of P-1,6-P-aldolase (91%).
Differential diagnosis of trichinosis
More than 40% of cases of trichinosis fall under the initial diagnosis: influenza, acute respiratory viral infections or acute respiratory infections.
Similar symptoms: acute onset of the disease, often with chills, high fever, muscle pain, lumbar pain, headache, pain when moving the eyeballs.
Differences: with influenza and acute respiratory diseases, a severe headache is usually localized in the area of the superciliary arches, symptoms of upper respiratory tract damage are more pronounced (runny nose, cough, hyperemia of the pharynx, nasal congestion, weakness, malaise). With these infections, muscle pain is less pronounced, there is no edematous syndrome and hypereosinophilia.
When differentiating trichinosis from typhoid fever and paratyphoid, it should be borne in mind that these infections are characterized by a more gradual development of the disease, inhibition of patients, anorexia, “typhoid tongue” – thickened and with dental imprints, lined with thick white or gray-dirty plaque in the middle part and free from plaque by the edges and tip of the tongue, the presence of a rose-colored rash in the chest and abdomen; the diagnosis is confirmed by the formulation of the Vidal reaction, RNGA, the allocation of the pathogen from blood, feces, urine.
With insufficiently careful and complete clinical laboratory examination, neglect of epidemiological data, the onset of trichinosis can be regarded as foodborne toxicoinfection or dysentery, and in children – measles, scarlet fever, tonsillitis, tonsillitis, etc.
One cannot also ignore the need to differentiate trichinosis from the acute phase of other helminthiases. In Ukraine, this primarily concerns an invasion such as opisthorchiasis, which in the acute phase can occur with similar symptoms. The differential diagnostic signs of acute opisthorchiasis are less pronounced muscle pain, edema syndrome, ocular pathology, but more pronounced abdominal syndrome and signs of diffuse liver damage: jaundice, hepatosplenomegaly, indicators of functional tests – increased bilirubin level, enzyme activity. The epidemiological history is of the utmost importance. Such epidemiological indicators as the group nature of the disease, when several cohorts fall sick after the festive celebrations, after eating pork meat, meat of wild animals, taking into account clinical indicators, are very important to justify the diagnosis.
Laboratory confirmation confirms the diagnosis. Laboratory methods for the diagnosis of trichinosis are divided into 2 groups: parasitological and immunological.
Parasitological methods are based on the possibility of detecting Trichinella larvae:
- in meat, which could cause infection;
- in a biopsy of the muscles of the patient:
muscle tissue (5-10 g), minced in a meat grinder, is placed in an Erlenmeyer flask containing artificial gastric juice in a ratio of 1: 20 – 1: 25 and kept in a thermostat for 3.5-4 hours. Then, after shaking, the contents of the flask are poured into test tubes with a capacity of 50 ml and sedimented for 30 minutes, after which the supernatant is carefully drained, and the precipitate is applied to slides and examined under a small magnification of the microscope.
You can use the method of digestion of biopsy material in gastric juice with the study of sediment after centrifugation.
It is empirically established that the number of larvae up to 200 per 1 g of muscle tissue corresponds to a moderate intensity of invasion, up to 500 – intense, more than 500 – super-intense;
o in some cases, to confirm the diagnosis on day 9-11 of the disease, a biopsy is made from the patient’s trapezius, deltoid or calf muscles. Under local anesthesia, observing the rules of asepsis and antiseptics, a piece of muscle 0.5-1 x 2-3 cm in size is cut out, from which thin sections are prepared between the glasses of the compressorium for microscopy. Trichinoscopy is also used for post-mortem diagnosis.
Immunological methods include:
- allergological techniques;
- serological methods.
Allergological diagnostic methods, with the exception of taking into account eosinophilia and an intradermal test, have not been developed and are not used in healthcare practice. The disadvantages of the intradermal test are its weak sensitivity and the possibility of additional sensitization of the patient’s body with the introduction of a trichinosis allergen.
Therefore, the methods of choice for the diagnosis of trichinosis are currently serological reactions with trichinosis diagnosticum.
In practice, a number of serological reactions are used: RSK (complement binding reaction), RCP (ring precipitation), RNGA (indirect hemagglutination), ELISA (enzyme-linked immunosorbent assay), RFA (fluorescent antibodies).
RNGA and ELISA are the most effective diagnostic methods, providing the detection of 80-91% of those infected, with specificity – 92-97%.
The simultaneous use of two reactions is recommended – RNGA and ELISA for greater verification of the result with the obligatory repetition of them (paired sera) after 2-3 weeks, taking into account the increase in antibody titer.
In the absence of specific anthelmintics in cases of mild to moderate severity, a complex of pathogenetic and symptomatic agents is prescribed. In cases of severe course, hormones are additionally prescribed. It must be remembered that with intensive invasion, treatment with glucocorticoid hormones is unsafe!